Spinal
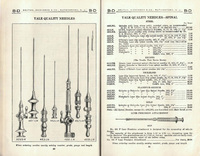
Becton Dickinson Gold Spinal Needle 462LNG, circa 1930
This antique gold lumbar puncture needle was framed and given as a memento to Leroy Vandam by AB Stearns around 1972. Why a gold needle? Dr. Vandam referred to gold as “anti-infection.” The Becton Dickinson Catalog of 1927 shows gold versions of their needles for sale.
Reports of success by August Bier (1861–1949), who attempted the first intentional subarachnoid block in 1898, (he used cocaine) led to the rise in popularity of spinal anesthetics in surgery. The subsequent, continuous experimentation worldwide led to safer alternatives to cocaine, better needle designs and insertion techniques. But, by the middle of the 20th century, with improvements in drugs and techniques for general anesthesia and a growing suspicion of potential adverse effects of regional anesthesia, (toxicity, paralysis…) the technique lost favor among anesthetists and surgeons. In 1954, Leroy Vandam, MD, Anesthetist-in-Chief at the Brigham, 1954–1979, co-published a study of 10,098 cases that proved its safety, causing a resurgence in the popularity of the “spinal.” The first ever, successful organ transplant (a kidney) which was achieved at the Peter Bent Brigham Hospital in 1954, was performed under spinal anesthesia. Vandam was the anesthesiologist.
Weiss Epidural Needle, contemporary example
Jess Bernard Weiss (1917-2007) was the Anesthesiologist-in-Chief at BWH predecessor institution, Boston Lying-in Hospital/Boston Hospital for Women, from 1961 to 1981, and was vice chairman of the Department of Anesthesia at BWH from 1982 to 1988. Under his leadership the Boston Lying-in Hospital slowly shifted away from inhalation anesthesia in favor of regional anesthesia for labor and delivery. Circa 1961, Dr. Weiss modified the Tuohy style epidural needle with the addition of “wings” which allows the anesthetist to use both hands to carefully place the needle, and blunted the tip to decrease the chance of accidentally puncturing the dura. The design of this tool for epidural anesthesia continues its worldwide popularity.
This needle is used to create an opening to the epidural space. The inner “stylet” prevents clogging the needle with tissue during the penetration of the skin. Once properly inserted, the stylet is removed and a thin catheter is inserted through the hollow needle. The stripes on the needle and catheter measure the insertion depth. The needle is removed and anesthetic can be introduced to the patient as needed through the catheter.